Laxmi’s industry-first dermal CGM, with a ~0-2 minute lag time between your actual glucose levels and the CGM’s displayed glucose measurement, is built for faster, safer decisions compared to legacy devices.
Current CGMs measure glucose in the subcutaneous tissue layer, where diffusion through adipose cells can introduce meaningful delays to the glucose reading.
Laxmi’s dermal CGM places a single, flexible sensor in the dermis, a richly vascularized tissue layer with minimal adipose cells, thereby enabling glucose readings that dynamically track much closer to blood glucose levels in real time.
Other companies utilize rigid microneedles (microneedle array) to access the dermal tissue space.
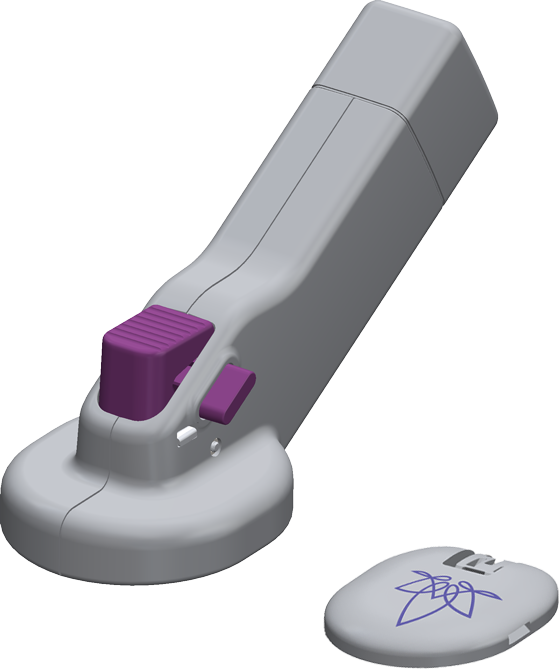
Shallow insertion depth of the sensor leverages the unique properties of the dermal layer of the skin.
Commercial CGMs penetrate deeper into the subcutaneous layer of the skin where physiology slows the diffusion of glucose from the blood to the sensor – creating time lag that can reach 10-15 minutes. The dermal layer is highly vascularized with a dense capillary network above and below the dermis which enables faster glucose exchange with the bloodstream.
The result: a significantly shorter lag time in glucose readings.
The deeper hypodermis skin layer (or subcutaneous skin layer) is mainly composed of adipocytes, with lower vascular density than that of the dermis. Glucose diffusion is slower in this deeper layer and results in a longer time lag in glucose readings.
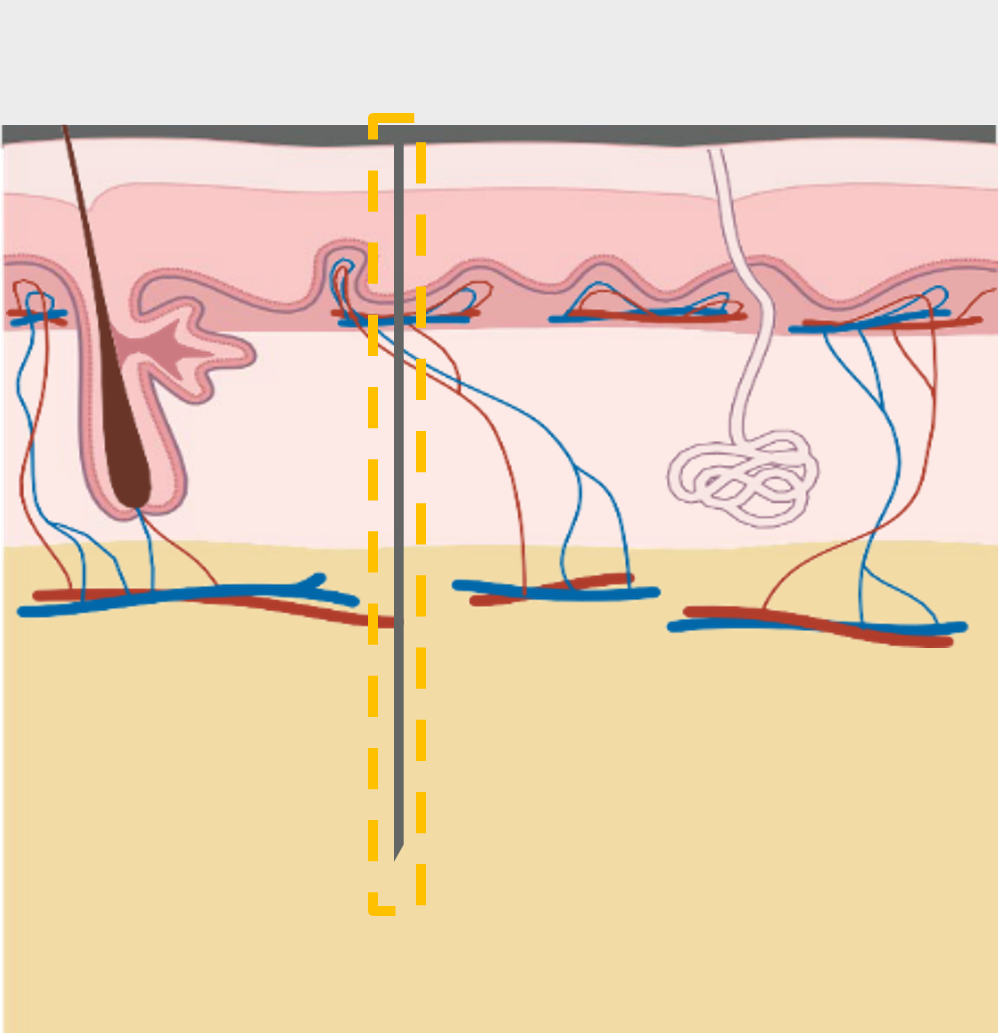
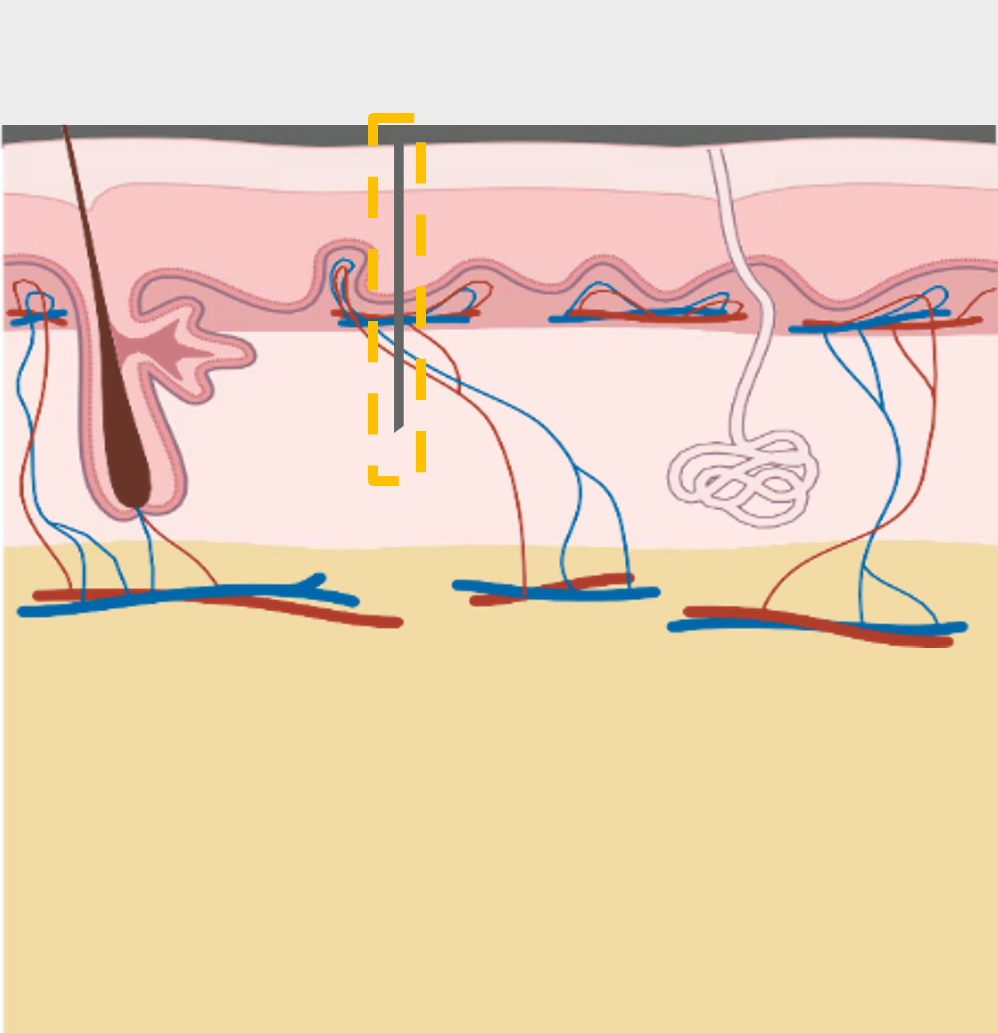
Laxmi's CGM enables dermal access with a single, flexible sensor, specifically designed to remain in the dermis throughout wear. Sensor insertion is facilitated by an applicator which employs a needle to quickly penetrate and then exit the skin leaving the sensor in the dermis.
Not a rigid microneedle and not a microneedle array
More consistent skin penetration, no risk of clogging micro channels, more signal stability
The dense capillary network and minimal to no adipocytes in the dermis help glucose equilibrate more rapidly – supporting far faster kinetics than subcutaneous sensing.
Current commercial CGMs compensate for the time lag of the subcutaneous tissue region by utilizing predictive algorithms that "look forward" to provide a glucose reading estimate.
In commercial CGMs, our clinical research data indicates a wide distribution of time lag across a range of 20 minutes (distributed around 0 with plus or minus 10 minutes). Negative time lag reflects the combination of filtering and predictive algorithmic signal processing.
The Laxmi CGM did not utilize any look-forward algorithms and achieved a time lag from 0–2 minutes for most sensors.
Tau = Time Lag. See more in our publication
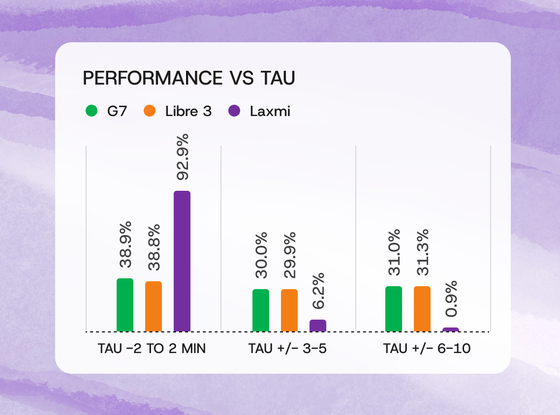
Laxmi’s dermal CGM achieved a time lag of 0-2 minutes (93% of sensors) while commercial CGMs showed wide variability, including large effective time lag distributions. The Laxmi sensor more accurately detected hypoglycemia conditions during clinical testing.
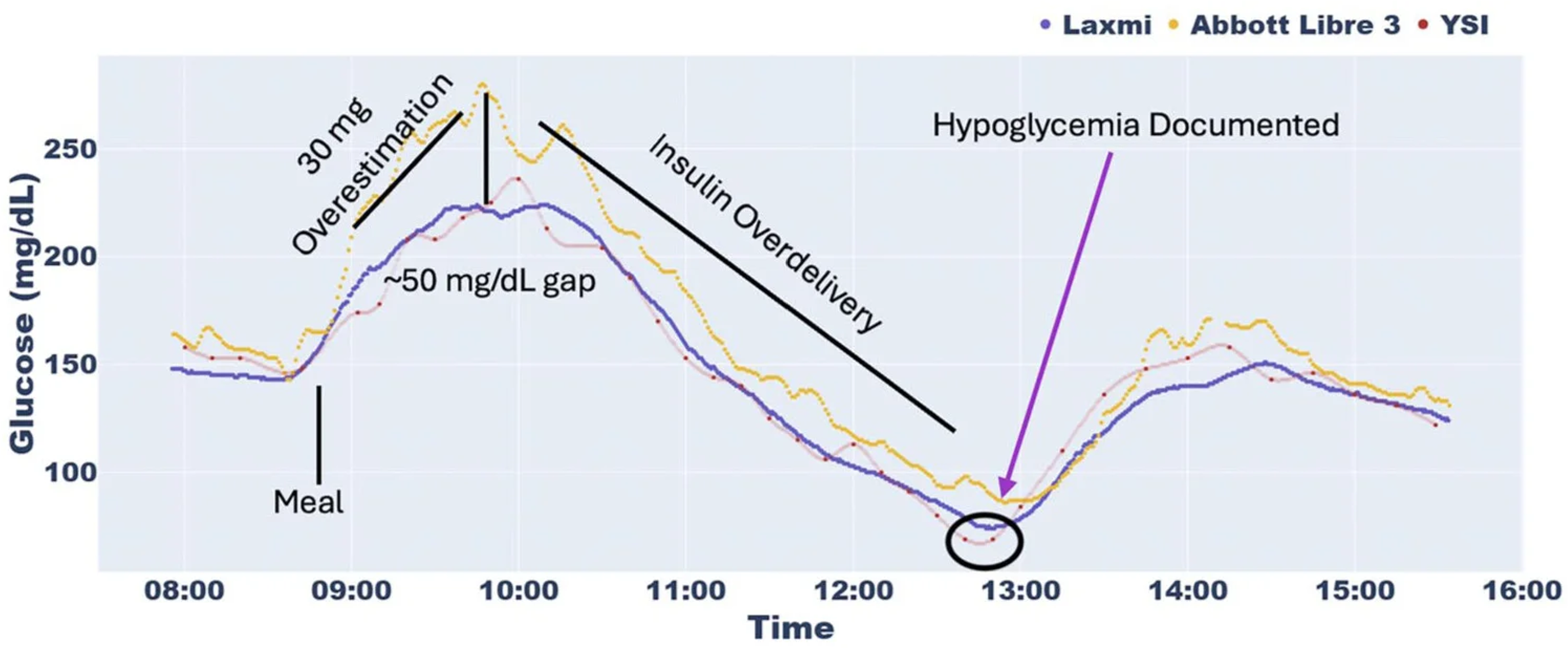
Laxmi’s dermal CGM achieved a time lag of 0-2 minutes (93% of sensors) while commercial CGMs showed wide variability, including large effective time lag distributions. The Laxmi sensor more accurately detected hypoglycemia conditions during clinical testing.
In clinical simulations, TIR dropped from 86% to 71% in adults when lag increased from 0 to 8 minutes.
With near-zero lag, patients and automated systems can respond sooner, reduce overshoot/undershoot, and potentially use lower glucose targets with less fear of hypoglycemia.

Clinical data has been collected during research studies (clinical trials) involving human participants (patients or volunteers).
Manuscript published December, 2025: Dermal Glucose Sensing has a Shorter Time Lag Relative to Blood Glucose: Implications for Hypoglycemia Detection and Time in Range
Presented October 28-30, 2025 at the annual Diabetes Technology Society Meeting, Burlingame, CA.
Presented June 19-23, 2025 at the annual American Diabetes Association Meeting, Chicago, IL.
Presented March 19-22, 2025 at the annual Advanced Technologies and Treatments for Diabetes Meeting, Amsterdam, Netherlands.
Presented October 15-17, 2024 at the annual Diabetes Technology Society Meeting, Burlingame, CA.
Presented August 7-8, 2023 at the BTIG Medical Technology & Digital Health Conference, California